The UK House of Lords Select Committee Behavioural Change Report was released on 19th July 2011. It’s an interesting read. However, more interesting is the transcript of evidence taken before The Select Committee that led to the report. In particular, a response to a question from Lord May of Oxford to Dr David Halpern about the analysis of evidence of efficacy of behavioural factors in the NHS. It revealed the size of backing given to behavioural research – or rather, the lack of it.
Professor Dame Sally Davies is the Director General of Research and Development and Chief Scientific Adviser for the Department of Health and NHS. David Halpern says
“[she] . . . sits on £500 million of research moneys, of which . . . we believe less than 0.5% of health research goes on behavioural factors . . . “
If behavioural factors make little or no difference – or perhaps 0.5% of a difference – to our health, than this is a fair distribution. Is this the case? Halpern continues:
” . . . and yet we know that more than half of all years of healthy life lost are to known behavioural factors . . . “
It’s a pretty big discrepancy, he goes on to say. Too right; 0.5% of the budget on factors that are likely to kill us in one-way-or-another is a pretty unfair distribution.
The question you should throw at me is ‘prove it’.
Why?
Because it can transform a hospital’s efficiency which is a benefit to both:
1. Those that use it because it is more efficient at the point of use
2. Those who don’t use it (but still pay for it though their taxes) because it is a more efficient use of every unit spent.
(For non-UK readers who are unsure of the NHS’s structure it is a nationalized health service, free at the point of use, funded by tax-payers)
Or, unhelpful if one wants to increase desire to stick to appointments.
Three appointments an hour, every day, for ONE MONTH; that’s a lot, right? A hell of a lot: four hundred and twenty ‘no-shows’ using a conservative
calculation. Therefore, no-shows must be prevalent, and – one can only infer from a large number such as this – are ‘approved’ by the group as a way of behaving. Must be: “We’re all missing appointments, I’m not so bad for missing mine, am I? The hospital are used to it . . . ” you’d think. Well, you would, wouldn’t you?
However, this is a strange truth.
Already, that changes thing’s a bit. But we can do better.
One month out of twelve is 8% of the total. Only 8% of appointments were missed, or, 92% of appointments were kept.
That’s even more powerful; all true, all real, all the same data. Let’s visualize that.
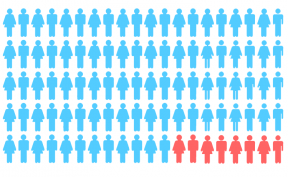
Eight out of every one hundred people fails to show for an appointment. Now, no-shows are not prevalent, and – one can only infer from a small number such as this – are ‘not approved’ by the group as a way of behaving. Can’t be: “Few people miss them, I’m an outsider for missing my previous one, they’re not used to it . . . ” you’d think. Well, you would, wouldn’t you?
(For comparison, In 2009/10 the total number of outpatient appointments missed totaled 6.7 million, or 7.9 per cent.)
Indeed, beyond appointments, behaviour sits at the heart of our health issues: Ralph Keeney’s paper in Operations Research cites deaths from individual’s choices increasing from 5% of deaths in 1900 to 55% in 2000; Dr David Halpern talks about the same. We’re not dying of disease and pestilence anymore – and the top killer isn’t cancer, heart disease, smoking, or overeating – we’re dying from the choices we make about our lifestyles (that have readily available alternatives).
The least we could do is make the communication interface in hospitals fall in favour of cost effective positive health outcomes.
(And we can start by marginalising missed appointments.)
For more on this speak with us, or have a look at our capabilities
Also, as co-founders and supporters of the London Behavioural Economics Network, join the Meetup group and Facebook group for more details and events
Related Posts
August 13, 2023
Money (but not called that, and how it changes behaviour).
Advertising agencies make a lot of…
August 1, 2023
Reading ease is not as easy as all that – comprehension shows the way
It's easy to make text readable, right?…
July 20, 2023
The ‘Hollywood hello’ – and the importance of context when communicating
When communicating we all like to be as…




